Career advice -- and commentary on current healthcare news and trends for savvy 21st-century nurses and healthcare providers -- from holistic nurse career coach Keith Carlson, RN, BSN, NC-BC. Since 2005.
Wednesday, December 29, 2010
A Red Scarf and a Cup of Tea
"That's OK. I remember you, and that's what matters. Nice to see you." I sit down at the table after she shakes my hand.
"I'm sorry I don't remember you, but you are very tall and handsome. Are you married?" She gives her ubiquitously flirtatious octogenarian smile.
"Yes, I've been married for 21 years." I take out my notebook and her client folder.
"Oh, too bad. I was hoping you'd stay with me." She sips some tea and folds her hands neatly in her lap again.
"Well, I don't think my wife or my boss would approve," I say, winking at her and getting out my blood pressure cuff and stethoscope.
"Did you have a nice Christmas?" I ask as I wrap the cuff around her arm.
"Oh, was it just Christmas? Oh, yes! I did," she says tentatively. "Thank you for asking." She looks confused.
As I inflate the blood pressure cuff, I watch her closely. Her respirations are normal---about 16 breaths per minute---and she seems at peace, but her mouth is quivering a little at the corner.
"Are you upset about something?" I ask, putting my supplies back in my bag.
"No, I feel fine," she says.
"Are you sure?" I ask again.
"Yes, I think so. I was upset about something this morning, but you know what?" She looks at me sharply.
"What?"
"I forgot what it was!" She laughs and drinks another sip of tea.
"Well," I say, "if you're ever upset about something, you can always talk to me."
"And what would I talk to you about?"
"Anything you like, my dear."
"Well, that's nice." She hesitates. "Are you going to stay with me?"
"No, I can't. But I'll be back next month, OK?"
"OK. Do you know what I forgot?"
"No, tell me."
"I forgot that Christmas is coming, and I didn't get my daughter anything." She begins to cry.
I hold her hand, and contemplate what to say. At this moment, the home health aide comes in, and intercedes on my behalf.
"You didn't forget your daughter, Mrs. ______. Don't you remember that we went shopping last week and bought her the red scarf? You told me she loved it."
My patient lets go of my hand, wipes her eyes, and looks up at the home health aide.
"A red scarf? You're sure?" She attempts a smile.
"Oh yes, I'm sure," the home health aide says. "You can ask your daughter about it later when she comes home. I think she's wearing it today."
"Oh, good. I thought I had completely forgotten. When is Christmas again?"
"It was last week, dear," I say, and the home health aide nods.
"Oh yes. That's right. Thank you." She sips her tea, wipes her eyes one more time, and it seems we've averted a crisis and an unnecessary dementia-related upset.
"Well, have a happy New Year, and I'll see you at the end of January." I take her hand and squeeze it gently.
"Thank you. I'm sorry you won't be staying with me. Are you sure you can't?"
I stand up and take my coat of off the chair. "No, I really can't. I have to get home to my wife. It's a holiday week and we have a lot to do. I'll be back to see you, though. I promise." I bend down to give her a hug, and she grabs the lapels of my coat.
"You're so handsome. Will you come back and see me on Christmas?"
"No dear, not on Christmas, but I'll be back soon. Happy New Year."
She smiles again, sips her tea, and picks up the paper. It's as if I've already left and she's forgotten that I was ever there.
I give the home health aide a hug and slip quietly out the door. Snow is falling again, and I look back at the house. My patient is sitting in the window, the picture of winter tranquility and coziness.
A red scarf, falling snow, a cup of tea, and the promise of a new year.
Monday, December 27, 2010
One Year Wanes, and Another Dawns
For me, this has been a year of great and momentous change. As most of you know, in October of 2009, my wife Mary and I sold our house and most of our possessions, left our beloved New England, and hit the open road in a 29-foot mobile home in search of intentional community. We chronicled that journey on our travel blog, Mary and Keith's Excellent Adventure, and in the course of our travels we visited more than 30 intentional communities in seven months.
Since June, we are settled---at least for now---in a lovely cohousing community in Santa Fe, New Mexico. Looking back, we readily acknowledge that everything we set out to accomplish has been realized: we live in a multigenerational intentional community with many like-minded souls, we are nearby to our son and daughter-in-law, our financial lives are more secure, we work less, we play more, and our quality of life is vastly increased. Speaking of counting one's blessings!
While we are uncertain of what the future holds, we currently have good health, a sense of belonging, a new coaching business, and there is a renewed sense in our lives that just about anything is possible.
As a nurse, I have two part-time jobs that are relatively non-stressful, allowing me more time to develop myself as a coach and as a professional writer. The nursing profession has been kind to me, and I relish being able to pick and choose the positions that are most suitable for me.
For this New Year, I wish all of you much success, health, abundance, love, prosperity, and a sense of peace in your hearts. Thank you for making Digital Doorway what it is, and I look forward to celebrating this blog's sixth anniversary with you next month.
Happy Holidays, Happy New Year, and my blessings to you and yours, now and always.
NurseKeith
Tuesday, December 14, 2010
Pediatric Nursing Article on WorkingNurse.com
Saturday, December 11, 2010
A Type of Suicide
During our chat, he pulled out a pack of miniature cigars and began puffing quite vehemently on one of them. I was surprised, and asked him why he smoked at his age.
"Well, I've been smoking two packs of these cigars every day for about 15 years and don't want to quit. I have a chronic cough that just won't stop, and I bust a rib every few weeks because I cough so hard."
I asked him if the coughing bothered him, and this was his reply.
"You see, I'm diabetic, so I'm not gonna live that long anyway. So why give up smoking now?"
I was shocked, and our conversation continued from there.
"Just a few minutes ago, you showed me some photos of your grandchildren," I told him.
"Yeah, that's right."
"Don't you want to live to see them graduate from high school? Don't you want to be there for them?"
"Hell," he said. "I don't control my sugars that good, anyway, so whether I smoke or not, I'm still gonna die. So what's the difference? I won't make it to their high school graduation no matter what I do."
Stunned into silence, I went about the business at hand, and I ruminated on what he had said. Basically, this man chooses to not focus on controlling his sugars, and he adds insult to injury by inhaling at least 10 of those cigars every day. Slightly overweight and sedentary, his ratio of body fat is also not doing him any favors. He is a walking time-bomb, and as he ages, his risk of blindness, amputations, kidney disease, and serious respiratory illness increases exponentially.
There are millions of Americans like this gentleman, millions of people who simply don't understand how (or why) to take care of themselves. Apparently ignorant of the proactive choices that they could make in order to halt (or even reverse) the forward march of their respective chronic illnesses, these individuals are destined for disability and/or institutionalization, costing taxpayers billions of dollars in health care costs that could have been altogether preventable had they willingly engaged in their own self care.
Nursing homes and hospitals are crawling with people who oftentimes make lifestyle choices that fly in the face of logic, poisoning their bodies with cigarettes, nutritionally unsound foods, excessive amounts of alcohol, and a sedentary lifestyle that certainly contributes to their eventual demise.
We are all footing the bill for people like my new acquaintance who simply choose to eschew their own well-being by pursuing a lifestyle that contributes to personal ill health as well as a society-wide health care crisis. When such a critical mass of people are drugged into oblivion by cigarettes, alcohol, TV, bad food and the mushrooming effects of ill health, it is a recipe for a nationwide disaster as well as a personal form of suicide.
Ben Franklin was prescient in saying that "an ounce of prevention is worth a pound of cure", but his admonition regarding the importance of prevention has apparently lost it's impact through the subsequent centuries. Most Americans seem to simply want a pill that will help them to eat less, quit smoking or lose weight, and that reliance on an outside source for the answer to one's personal health concerns is misguided and serves as a poison in the veins of the society.
Our health care system is in crisis, and our population is aging and growing more obese and ill with each passing year. As costs rise and quality of care decreases, a small few profit from the mess as most of us suffer the collective consequences.
The smoking diabetic described above is one of millions of Americans who choose to take the path of least resistance when it comes to their health, and if I explained to him that his choices are actually driving up the cost of health care around the country, he probably would have looked at me as if I had two heads.
Americans may be obsessed with health on one hand, but on a very deep level we seem to have basically given up the ghost. My diabetic acquaintance certainly sees no reason to change any of his habits, and as he slowly commits suicide, his care will consistently tax the system, adding to the sorry statistics that paint a picture of American health care that is anything but rosy. His premonition that he won't live to see his grandchildren's high school graduation is probably accurate, and when his grandsons wonder why Grandpa couldn't be there to watch them accept their diplomas, will anyone use his story as a cautionary tale? Most likely not, and the cycle will probably repeat itself in the next generation in a form of suicide that is, for all intents and purposes, more common than any of us would like to believe.
Sunday, December 05, 2010
Cold Comfort
Although hospitals offer an essential service, they can often be comfortless, cold and unwelcoming places that are polluted with noise, unnecessarily bright lights, the constant interruption of patients' desire to rest, and a dizzying array of providers with whom patients sometimes have little or no personal connection as they are poked, prodded and otherwise examined.
Observing my father in his room in the rehab facility, the first thing I noticed was the fact that he was being constantly barraged by noise that intruded on his well-being and his ability to rest. Staying in a two-person room, a patient is always subject to the vicissitudes of having a roommate, and my father was unlucky enough to be at the mercy of his roommate's intermittent groans of pain and complaint, and also the high volume of his television that was on from the moment he woke up in the morning until he turned out the light at bedtime.
To add insult to injury, nurses and aides laughed and talked loudly in the hallway, carts with squeaky wheels were pushed down the hallways at all hours, and intercoms and buzzers continuously added to the nauseating medical din.
My father, sitting with his head in his hands, accepted the offer of foam earplugs procured from the nurses station, but they sadly did little to block out the constant noise that infiltrated his world and rattled his already troubled brain. The poor guy just wanted to rest, and the very facility promising him "healing" offered an environment completely unsuited to that end.
In my mind, most hospitals, nursing homes and health facilities are built with the convenience and ease of its employees in mind. While the physical layout does indeed need to take the efficiency of health care delivery into consideration, the lack of consciousness around patient comfort is nothing short of appalling.
When it comes to noise pollution, every patient bed should be equipped with wireless (or wired) headphones connected to the television, eliminating the cacophony of two televisions tuned to different channels blaring simultaneously in every room.
Next, every cart and wheeled conveyance used in a health care facility should have the most state-of-the-art solid rubber wheels that provide the most silent movement possible. From mop buckets to gurneys, wheels should be as silent as a whisper.
Regarding nurses and other staff, voices should be as quiet as possible, and while laughter and joviality provide for a more lighthearted work environment, I have observed that many staff frequently seem oblivious to the fact that their place of work is also a place where patients come for rest and healing. Staff do not need to take a vow of silence, but conversational voices can convey information more readily and efficiently than raised voices loud enough to wake the dead.
And then there are the lights and the environment. Where are the full-spectrum bulbs, skylights, picture windows, fountains, options for soothing music, and views of the outdoors that are conducive to healing? Why are rooms not designed in a manner wherein each looks in upon a central courtyard of beauty? Where is the research on the use of color and light to induce a feeling of calm? So many hospital walls are adorned with awful colors reminiscent of the dull and uninspiring hues of vomitus and stale urine. Hospitals are not meant to be prisons.
Watching my father react to the noise, interruptions, bright lights and cheerlessness of the hospital and rehab facility, I was struck by the readily visible fact that many facilities simply ignore the creature comforts of patients, creating environments that neither inspire nor engender restful recovery. Feeling powerless to help him to be more comfortable, my visit came to an end, and it was little comfort leaving my poor sick father at the mercy of an environment ill-suited to his overall well-being.
While there are indeed some superlative hospitals out there that embody the very heart of the nature of the healing environment, most mainstream hospitals offer a pedestrian and uninspiring atmosphere that does little to assist the sick in their process of recovery. Those hospitals that do provide optimal care and a healing environment should be held up as an example to those who simply take the path of least resistance.
Leaving my father sitting alone in that rehab was one of the hardest things I have ever done, and I hope to never again be in the position to leave someone behind who is receiving care in a facility in which I do not have the utmost confidence. While there was one nurse who took a special interest in my dad, that was cold comfort in light of the suffering that he was experiencing, and I'll sleep better when he is safe and sound in his own home once again.
Wednesday, November 24, 2010
Cielo
She looks up at me from her seat next to the window.
"I'm the nurse and I'm just coming by to check on you. Besides, I'm married, and my wife wouldn't like it if I didn't come home." I sit down next to her on the couch.
She laughs. "What's your name again, my dear?" she says in Spanish.
"Keith," I repeat, for the third time in five minutes.
"Is it Christmas this week?" she asks. "Will you bring me a present?" Again in Spanish.
"No," I answer in Spanish this time. "This Thursday is Thanksgiving. Christmas is next month."
"Oh," she says, and takes my hand in hers. "Are you staying with me?"
"My dear," I reply, "I'm the nurse, and I'm just here for a few minutes. It's so nice to sit with you here and chat."
"What's your name again? You're so handsome!" She smiles at me.
"I'm Keith, and I'll be back to see you again next month, OK?"
"OK." Another smile.
We sit for a long minute or two, her hand in mine. Her live-in caretaker is frying eggs and sausage. The smell fills the room and I'm suddenly hungry. I think about stopping for a cup of decaf on my way to see my next client. Decaf with honey and cream.
"What's your name, dear?"
"It's Keith, cielo, and I'll see you in a month or so. Enjoy your breakfast and happy Thanksgiving." I stand up from the couch and I feel like a giant next to her small frame huddled on the couch below me. She seems Lilliputian, simply diminutive.
She looks up at me with wide eyes, her mouth open and smiling. I lean down and give her a kiss on the cheek. It's a risk since it's the first time we've met, but she's been flirting with me since I arrived, and a kiss on the cheek seems appropriate and safe. Her caregiver looks up from the stove and smiles.
"Happy Thanksgiving, dear," she says in Spanish.
"Happy Thanksgiving, cielo," I say in Spanish. ("Cielo" is "heaven" or "sky" in Spanish, and it's used as an affectionate term of endearment.)
I walk outside, and I look back at the window. She's holding the newspaper in front of her face, scanning the words and shapes in front of her. Can she understand what she sees? Probably not, but she's happy, clean, well fed, comfortable, and we had a thoroughly lovely visit.
Happy Thanksgiving, cielo.
Wednesday, November 17, 2010
Caffeine + Alcohol = Danger
A new study has already revealed that beverages containing high levels of caffeine can increase dependence on alcohol, and some data reveals that young people who regularly use energy drinks are more likely to indulge in binge drinking and high-risk behavior.
Beverage companies have recently gone out of their way to create products with catchy names like "Joose", products that are packaged in a flashy manner that belies their questionable and unhealthy contents.
While super-caffeinated drinks like "Red Bull" have been popular for years, newer drinks containing very high doses of caffeine coupled with a 12% alcohol content by volume bring a new problem to the fore. The FDA and other groups have found that young people under the influence of these volatile caffeine-alcohol mixtures are less likely to feel the effects of the alcohol that they are imbibing since it is mitigated by the excessive amounts of caffeine being ingested simultaneously. So, these individuals drink more and more, putting themselves at risk not only of alcohol poisoning but also from the cumulative effects of the stimulating herbs and amino acids contained in these beverages.
Many young people will no doubt feel that the government is overstepping, intruding on their ability to purchase products that are inherently legal yet contain dangerous mixtures of substances whose combination (and excessive use) create enormously dangerous situations.
As I write this post, the FDA has issued a warning to the manufacturers of caffeinated alcohol drinks that the products must be removed from shelves and reformulated. Meanwhile, many universities and colleges---along with some states---are banning these products of their own accord, and we can probably rest assured that energy drinks will continue to come under close scrutiny by parents, consumer groups, the FDA, and researchers.
In a country where the market and profits rule, manufacturers have taken advantage of the situation by marketing products that endanger the health and very lives of vulnerable (and frequently naive) young people. Just like the cigarette industry (which set such a nefarious example), these companies are, as usual, putting profits before safety and health, peddling unregulated products that feed the American addiction to speed, pleasure, and consumerism, not to mention the proclivity towards alcoholism and substance abuse.
The FDA took a stand this week, and I deeply hope that they will follow through on their actions further holding the beverage industry accountable for such a wanton display of poor judgment and corporate selfishness. Our young people don't need companies to hand them their own demise on a silver platter (or, rather, in a seemingly innocuous and brightly colored can), and we need the FDA and other regulatory bodies to walk their talk when it comes to protecting the public from products that create such utterly avoidable scenarios of danger, ill health, and reckless choices.
Wednesday, November 10, 2010
Pondering Loss, Gratitude and Life
That said, Autumn is often a time of loss for many of us. We grieve the death of Summer, the death of the warmer weather (if we live in an area with normal changes of season), and we either embrace or resist the coming Winter and the more internal hibernatory nature of the colder months.
For me, this Autumn certainly brings with it a sense of loss as Summer wanes and Winter begins to take hold. It also brings to mind past losses and future losses yet to be.
One year ago, my wife and I pulled up stakes in Western Massachusetts, sold most of our belongings, and set out on the open road in a used mobile home that we purchased as our ticket to freedom. That leave-taking was difficult after twenty rich years of life in one place, but it seemed like the right time to leave, and we seized the moment.
Not two weeks after our departure, a dear friend took his own life, forcing us to return to New England in order to mourn his sudden death. This week marks the one-year anniversary of his last desperate and violent act, and the falling leaves and chilly air conjure images of a cold November day last year when thirty of us stood outside the barn where he had hung himself, sharing stories of our dear friend David.
Now, another friend on the East Coast is battling metastatic ovarian cancer, and her poor prognosis and continuing decline give us pause as we note her long-standing importance in our lives and the distinct possibility of losing her.
As I write this post, my eighty-year-old father (who was, by the way, loathe to celebrate his 80th birthday for fear of what this new decade would bring) is beginning what seems to be a slow decline, showing signs of early Alzheimer's, physical weakening, and a general diminishing of the childlike and optimistic spirit that has been his lifelong calling card.
Just this afternoon, a neighbor underwent surgery, and although she is young, healthy and vibrant, it is yet another reminder of the transient nature of our bodies, and the risks we all run by simply being incarnate human beings.
I am grateful for this life, for the people and animals who inhabit it, and I am again and again reminded how, by the grace of God, I continue to be a healthy and intact person who has a roof over his head, money in the bank, food to eat, clothes on my back, a car to drive, and an abundance of loving people around me. It is no small miracle, and the ubiquitousness of loss and death are yet another reminder of just how lucky I truly am.
As David's spirit continues on it's journey and as our dear friend grapples with the cancer that may eventually end her life, I am cognizant of my own continued blessings and how they are not to be taken for granted.
The mysteries of life are legion, but the importance of appreciating that mystery trumps every petty complaint and worry that crosses the mind. For me, the greatest lesson is the need for consistent gratitude, even in the face of loss and grief. It is a steep learning curve, yet one well worth the effort and energy to surmount in the hopes of experiencing peace, acceptance, and the knowledge that life is a gift never to be wasted.
Saturday, October 30, 2010
Working Nurse: Emergency Nursing
Wednesday, October 27, 2010
Haiti, Cholera, Water, and a Crisis
With the cholera outbreak making itself known in the streets and slums of Haiti, we are again reminded how those of us living in various industrialized nations take sanitation, health, clean water, and access to proper medical care for granted.
Here in the United States, an outbreak of cholera would be as unlikely as a massive epidemic of bubonic plague. But in the case of Haiti, deplorable conditions pre-dating the relatively recent earthquake have created a situation wherein otherwise preventable diseases can spread rapidly and dangerously from rural to urban areas (and back again) in a matter of days.
In the Western Hemisphere, Haiti remains a symbol of failed economic policies, illegal coups, and inappropriate interventions by the United States and other global bodies who have crippled this poor nation and left its citizens lagging behind as the poorest country in this half of the world, with the majority of its 9 million citizens living below the poverty level.
International aid organizations, many of whom have had boots on the Haitian ground for decades, are now scrambling to provide education, outreach and improved sanitation in order to head off an outbreak that has already killed hundreds and could very well kill thousands if the tide is not quickly stemmed. Some groups, like Doctors Without Borders, are building makeshift cholera clinics, and others are distributing chlorine tablets for the purification of water and oral rehydration fluids for those at risk of dehydration in the absence of clean drinking water.
Newly living in the American Southwest, I’ve recently been learning how contentious an issue water has become in the 21st century. Native American tribes have been forced to utilize the courts in order to gain access to water to which they previously had the rights for generations, and just a few weeks ago, bloggers worldwide participated in Blog Action Day, this year focusing their attention on water as a global issue of critical importance.
In Haiti, an economically crippled country was only recently brought to its knees by a massive earthquake that left more than a million homeless Haitians living in various tent cities as they await a more permanent housing solution. According to reports, sanitation and hygiene is actually worse in the urban slums, where water used for drinking and washing is contaminated with fecal matter, proliferating the spread of diseases such as cholera.
As some of us here in the Southwest argue over how many rain barrels we can afford to buy in order to have enough water to irrigate our decorative gardens, millions of Haitians long for the opportunity to simply have sufficient water to provide proper sanitation, healthy hydration, clean and hygienic clothing, and irrigation for life-sustaining crops.
In this world of plenty, Haiti’s current state is a sign that the priorities of the human race are tragically askew. Meanwhile, the conspicuous consumption and epidemic obesity of those of us in the industrialized world only further illustrate our loss of a collective vision of how life should be for all.
Haiti needs our assistance, our empowerment, and our generosity. And we can only hope that, given time and adequate resources, the poorest country in the Western Hemisphere will one day be relatively free of disease, poverty, and the misguided geopolitical interventions of those who have only sought to exploit her.
Friday, October 22, 2010
Nursing Shortage Infographic
--------
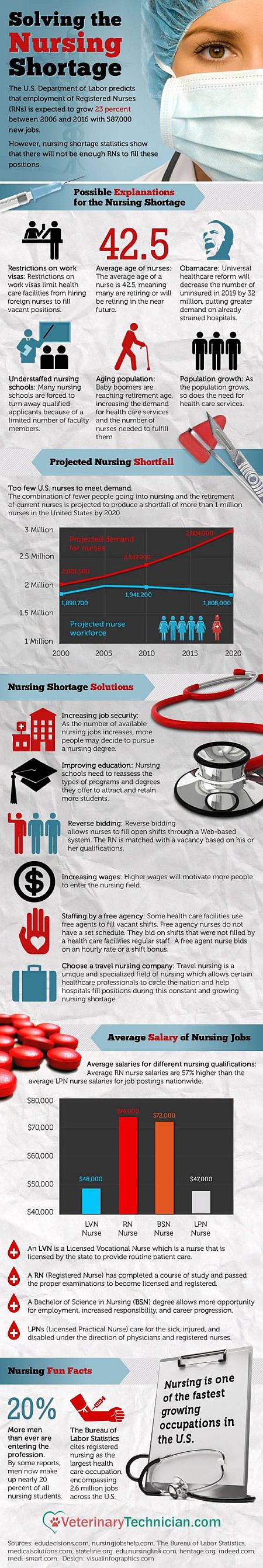
Via: VeterinaryTechnician.com
Friday, October 15, 2010
Global Handwashing Day and Blog Action Day
Every day, more than 5,000 children die from diarrhea, and this is largely due to lack of access to clean water and soap with which to practice hand hygiene. And over all, 42,000 people die every week from lack of access to clean water. With more than a billion people worldwide (that's one in eight human beings) lacking access to clean water, the proportions of this issue are staggering and the implications for public health, disease management, economic development, food production and simple survival are staggering.
From the dual perspectives of Blog Action Day's theme of water and Global Handwashing Day's emphasis on clean water to facilitate handwashing and the prevention of disease, there is a natural symbiosis. With drought and desertification becoming an increasing global problem, action is needed on all fronts to combat this issue and turn the tide, so to speak, on the global water crisis.
Here is the Blog Action Day YouTube video which is well worth watching for a quick synopsis of the movement's mission:
And please watch this video from The World Bank, and feel free to visit the Global Handwashing Day website to get involved.
Sunday, October 10, 2010
A Grateful Kiss
Her husband dotes on her with devotion and love, and though they both tire of the struggle from time to time, there is nothing to do but continue.
Although she cries every few days, most likely out of frustration, her smile can still light up a room, and her eyes sparkle with a keen intelligence and wit that she simply cannot express with language.
I have visited three or four times now to check on her and the assistance that the home health aides provide, and our connection becomes sweeter with each visit. At first, I would hold her hand as I talked with her, looking into her eyes, making as much contact as possible, always talking to her rather than talking about her in the third person. Her husband, standing nearby, observes our interactions and obviously approves.
This past week, I felt a compelling urge to give her a hug as I prepared to leave after a brief visit, and she made it very clear that only a kiss would do. Surprisingly, she kissed me on the cheek with gusto, hugging me tightly with her good arm, and as she let go, she beamed me a smile that would melt the coldest heart. It was one of those moments in life, and the gratitude and love in her eyes is something I will always remember.
This courageous woman and her husband daily continue the work of recovering the functions that were lost when the massive stroke tore through her body like a bolt of unfortunate lightning. Locked in her brain and unable to verbally communicate the feelings and thoughts that swirl in her mind, her deep hazel eyes still well with emotion, and she does indeed communicate in myriad ways.
Visiting this lovely woman and her husband is a pleasure, and on this particular day, she bestowed on me the gift of unabashed affection with a simple kiss and hug, and I left their cozy home radiant with delight and gratitude for the reward of being the nurse for such a courageous and wonderful woman.
Friday, October 08, 2010
More Articles at WorkingNurse.com
My Specialty: Oncology Nursing
My Specialty: Nursing Informatics
My Specialty: Home Health and Hospice
Disaster Relief Nursing
Thursday, September 30, 2010
Of Oatmeal and Mass
"How are you?" I ask as I sit down on the seat opposite the couch where she spends her days and nights.
"Fine," she says, looking at the floor. She fidgets with the hem of her dress.
"How are things going with the home health aides? Is there anything new you need them to do for you?"
"No. It's fine." She fidgets some more.
"How are you sleeping these days? Do you get enough sleep?"
"I don't sleep too well. But I'm fine," she replies. Her lack of eye contact is unnerving and I fumble for ways to make a deeper connection, but this is only our third meeting and I know she needs time to build trust, so I'm patient.
"Is there anything I can do for you? Is there anything you need?"
"No, I'm fine." She looks over at the TV. "Mass starts soon and I still have to make my oatmeal."
The clock on the wall ticks and tocks in the silence between us.
"Your house looks lovely. You take such nice care of it. Have you lived here a long time?"
"My husband built it forty years ago. Every board and nail. He even did the adobe. We raised our children in it, and he died nine years ago." Her affect brightens as we look around the house.
"The woodwork is beautiful, and I love the counters in the kitchen. He did a brilliant job," I add.
"Thanks," she smiles.
"I really have to make my oatmeal now. I don't want to miss Mass."
"OK," I say. "I'll come by and see you at the end of October, and I hope you have a good month til then." We shake hands.
I open the front door and light comes streaming in. She squints, shades her eyes, and says goodbye as she closes the door. Mass and oatmeal await.
Friday, September 17, 2010
Change of Shift, Vol. 5, Number 6
I'm pleased to again be included as a contributor, and my thanks as always to Kim at Emergiblog for being a champion of nurse bloggers around the world. Kim has worked tirelessly to promote the many nurse bloggers who pour out their hearts and souls to describe the joys, frustrations, challenges and rewards of the incredibly varied profession of nursing. She remains ahead of the virtual curve, and inspires us all to continue writing and sharing our experiences with the world.
Tuesday, September 14, 2010
Ashes to Ashes
Stopping in my tracks, I approach the box, my mind flashing back to the day when I picked up my step-father's ashes from the funeral home, overwhelmed by the fact that his 72-inch tall body weighing 180 pounds in his prime was now reduced to a box of detritus weighing in at less than 10 pounds. I recall driving home with that box in the passenger seat of my car as I cried in relief for the end of his suffering, despite the surreal notion that all that was left of his physical body now fit in a small container that bounced nonchalantly on the seat as I raced towards home.
Returning to the present, I gently opened the white box bearing my deceased patient's name, and reached in to grasp in my hand a clear, thick plastic bag containing her remains. I lifted the bag out of the box, weighed it in my left hand, and closely examined the small chunks of bone interspersed in the grayish ash. Closing my eyes, I conjured her face in my mind's eye and sent her a prayer of comfort as I returned the bag to the box and closed the flaps tightly.
I had only met this patient once, and although I had heard that she was dying, my next visit was not scheduled quickly enough, and she died before I could make a final visit. Our agency's home health aides knew her well, providing intensive personal care as her illness progressed. An intellectual, writer and retired professor, her body and mind had deteriorated greatly over the last five years, and those who knew her well understood that this mental and physical deterioration had been incredibly difficult for her to accept. Unable to read, write or speak, she was trapped in a body that had become, for all intents and purposes, a vestige of itself, a shell almost entirely incapable of personal expression. Despite having no living family, she did not die alone, and this is a comfort to all who knew and loved her.
Leaving my supervisor's office, I was flooded with memories of my step-father and his final days, especially that last day of his life when we all gathered around his bed to witness his last intake of breath. He never exhaled, and it was as if the six of us expectantly gathered around his bed had exhaled for him, sending his spirit out from his body on its journey into the unknown.
Next, my old dog Sparkey came to mind, and I pictured that day in late summer when the vet came to our house and assisted him to leave his pained and wasted body behind. As the medication entered his veins, he licked each of our faces in turn and a single tear ran down his furry cheek. It was a difficult goodbye, but his suffering was due for a humane and timely end.
Now a dear friend of ours struggles with cancer as she grapples with what treatment regimen will be most effective and least toxic, and her phone messages and our conversations across the country reflect the potential of loss that we are all facing vis-a-vis her mortality.
Recently, another dear friend's sister took her own life, and another acquaintance died after a brief but heroic battle with leukemia.
That little white box and its contents of ash and pulverized bone were a provocative reminder, a physical and unexpected talisman of the final ride that we all must eventually take. Bearing this in mind, I considered my own complaints and their relative pettiness, and was once again reminded of what a brief and wonderful privilege it is to inhabit a human body, walk the earth, and breath in the air of life.
We arrive to this world empty-handed and leave with nothing but our soul. They say you can't take it with you when you go, so we have to make the most of this fleeting earthly sojourn of ours. I am grateful for the time I have, and when it's my turn to take my place in a little white box of ash and bone, I will do so with gratitude and the knowledge that this was a life well lived.
As the saying goes, ashes to ashes.
Sunday, September 12, 2010
Cookies
"After ninety-five years, I figure I have a right to be lazy."
"So," I responded, smiling, "what does old and lazy look like to you, my dear?"
"Well, I get up in the morning at my leisure, take my time getting washed and dressed, sip on some coffee, look out the window, and eventually make my way to the living room or the patio. Sometimes I eat lunch, sometimes I don't, and then the rest of the day I can do whatever I want, really." She sips some coffee and has another bite of a cookie, offering me one from the plate.
Taking a cookie, I bite into it as we look into each other's eyes and smile, sharing the simultaneous experience of the flavor of the cookie, the brilliant New Mexican light, and the fresh September breeze coming through the dining room screen door.
"Do you feel like your needs are being met? Are you happy with the care you're receiving? Is there anything you need?" I put my cookie down on the plate in front of me.
She looks very thoughtful. "After so many years, I have no complaints. It's been a wonderful life. My kids love me and care for me. You people come to help me. The house is beautiful and I can see the sky and the mesa out there." She points vaguely towards the window. "I'm happy. I really am."
We each take another bite of a cookie, and she pats the head of the family dog who has buried his head in her lap.
"Have another cookie," she says, and smiles.
Friday, September 03, 2010
Change of Shift, Vol. 5, Number 5
Wednesday, August 25, 2010
Did I Miss Something?
When I arrived, she was supine in bed, the home health aide by her side. Questioning her, I could perceive nothing more than neck and leg pain, something that the orthopedist had recently confirmed as being caused by worsening chronic osteoarthritis.
"Have you been taking your pain medicine?" I asked.
"Not really," she replied. "I don't like to take that stuff." She made a face.
"Well, you might want to think about taking it at least a couple of times a day when the pain is this bad. You might not like taking it but it may help you to feel a little more functional."
"Maybe you're right. I'll try it and see how it goes. They're sending me to the pain clinic, anyway."
I did a thorough head to toe exam. She was neurologically intact, her bowels were normal, her urinary function was normal, and her lungs were clear. All vital signs were perfect. She denied reports that she had vomited the day before, but her mild dementia could be the reason she couldn't remember. Checking the home health aides' notes, I realized that no vomiting had been documented, so who knows if it happened or not? A few recent falls were documented though, and the bruises on her shin and ankle told the story.
"Did you hit your head when you fell? Was it scary?"
"No," she replied. "Not particularly. I caught myself but I knocked down a lot of papers and magazines in the process." Her house is covered with piles of mail, papers and magazines that the aides are constantly trying to reduce. As if to illustrate that fact, the home health aide made a move to retrieve the bottles of medications from the bathroom, and yet another pile of magazines cascaded to the floor. We both stooped to pick them up as our client watched from her bed.
Sitting on the edge of the bed and chatting with my client and the home health aide, I evaluated her speech, made certain that her facial features seemed even and smooth, and had her push her feet against my hands to test her strength. All reflexes were normal, her grip was strong and even on both sides, and I could see nothing wrong aside from the chronic pain that has dogged her for years. I was perplexed that the home health aides had made the assessment that she was acutely ill.
"Well, I know you're not scheduled to have an aide on Saturday and Monday, but I'm going to recommend that you have daily care for the next week, at least until you feel a little bit better and can see your primary doctor and get that referral to the pain clinic." I began to pack up my things.
"OK. That sounds fine. It's just so frustrating to be so limited. The pain is horrible, and I'm lonely."
I held her hand, chatted for a few more minutes, and took my leave. The home health aide was going to stay an extra hour, and I called the office to have daily care approved for the coming week, and drove home to continue my day off.
The next day, my supervisor called to tell me that the morning aide arrived to the house, let herself in, and found our client dead in her bed, reclining in the same position in which I had left her the day before.
I was shocked at the news, and immediately began to question my assessment. Had I missed something? Was there a clue I had overlooked? Was I remiss at not sending her to the emergency room? Would my skills and license be brought into question?
There has been no answer as to the cause of death for this woman who appeared, for all intents and purposes, to be suffering from chronic pain, loneliness, and a slowly progressing dementia. I am certain that my assessment was accurate and that she was not acutely ill that day when I was called to her home to assess her. Still, the questions linger, and they are most likely questions that will never be adequately answered.
May she rest in pain-free peace.
Saturday, August 21, 2010
Change of Shift, Vol. 5, Number 4
Monday, August 16, 2010
Of Birthdays and Death
As a nurse, I have worked with the dying and the chronically ill for many years, and their struggles are a reminder that our hold on this mortal coil is tenuous, at best. Several years ago, my wife and I spent about three weeks living at my mother's house in New Jersey, caring for my step-father as his body slowly diminished in its power and presence at the hands of pancreatic cancer. Presiding over his dying process and his death was a powerful and moving experience, and despite my many years of nursing, his was the first death that I witnessed firsthand. That last gasping intake of breath was profound in its finality, even as we waited for the exhalation that never came. I noted how quickly the life force left the body, and how quickly we shifted from care-taking to grieving in the space of one breath.
In 2001, a very close friend of our family was gunned down by the police in a circumstance that might be plausible in a movie or novel, yet was wholly unreal to those who witnessed it and those who survived his horrible passage from this world to the next. Distressed, he had called our home to solicit our assistance moments before the police burst in and riddled his body with seven bullets, and we heard his dying cries of love on our answering machine as he lay bleeding. His death was indeed something almost beyond belief, and the post-traumatic stress that followed was life-altering.
Last year, a dear friend took his own life after years of struggling with chronic pain, depression, and an undiagnosed cognitive condition that robbed him of the ability to use his brilliant brain in the way in which he was accustomed. Memory failed him, words were slow to come, and the loneliness that he experienced was simply too profound for him to see a way to continue on. His 51st birthday would have been last Friday, and I miss the opportunity for him and I to celebrate our August birthdays together, Leos in heart and spirit.
Another close friend was diagnosed with an advanced cancer a few months ago, and this shocking news of urgent surgery, treatment and the potential for death from the ravages of the disease were yet another wake-up call. She is literally fighting for her life while she also faces her own mortality square in the face with courage and understanding that our time on this earth is indeed limited, either by illness, fate or irreversible circumstance. She is a shining example of grace and courage in action.
The other day, it was revealed that a close friend's sister died suddenly at 42, leaving a young daughter without a mother and a confused group of family members and friends. Sudden death is perhaps the most difficult to digest and understand, but acceptance is still the eventual goal, no matter how challenging the path to that state may be.
So, birthdays come and birthdays go, and we move forward in our lives with our petty complaints, our desire to do better, and the courage to continue on even in the face of monumental loss and grief. Birthdays are indeed a time for celebration, but they are also a moment for reflection, atonement, and the realization that this very birthday may very well be our last.
In light of that reality, why then do we waste such precious time with the minutiae of our complaints, problems and apprehensions? This is one of the puzzles of human life, and perhaps this year I will learn even more deeply that my time on this earth is limited, that these days are precious beyond description, and that it's time to live life without regret and hesitation. Perhaps this is the year when I will realize the enormity of the gift, embracing life with the open-eyed wonder that its many mysteries deserve. Happy birthday indeed.
Monday, August 09, 2010
Change of Shift, Vol. 5, Number 3
Saturday, July 31, 2010
We're All in This Together
She sits in her chair most of the day, looking forward to happy hour at five. She's lived a good life, and there's nothing that will change her habit of drinking a bourbon and water (or two) at the end of each long afternoon. Nearing 100, she's even taken up smoking a cigarette with her bourbon, and there's nothing that will change that, either.
"I never expected to live this long. Who could have imagined it?" she says with apparent sincerity. And when questioned about the new habit of smoking, she says, "And why not?" with a smile.
"My life has been lovely, my children are wonderful, and I have no complaints other than my loss of mobility. Still, life is good and my days are my own."
I inspect her toenails and decide that a podiatrist should be the one to tackle their impenetrable thickness. Her ankles are without swelling, her abdomen is soft and non-tender, and her cognitive functions are intact. Her vital signs are stable, her pacemaker works like a charm, and her positive attitude certainly makes up for the deficits that have significantly reduced her independence.
"Life has been an adventure, and now I get to sit in this chair, look out at this wondrous view, and have myself a nice stiff drink at the end of the day."
Her daughter winks at me knowingly, and acknowledges in a whisper that there's now more water and less bourbon than ever at happy hour.
"Well," I say, "I wish I could make up excuses to stay here all afternoon and chat, but you're doing so well there's nothing more to say. I'll come back in a few months to see how things are going with the home health aides. Call me if you need anything, OK?"
I shake her hand, but it's apparent that she wants a kiss, so I lean down and peck her on her powdery cheek. She smells like lemons.
"Thank you, dear," she says. "Please come back soon, and don't just wait til they tell you that you have to come back. The door is always open." We smile at one another widely as I exit her immaculate bedroom.
"She's a wonderful woman," I say to her daughter as we walk to the driveway. "She's lucky to have you and your brother."
"Yes, she is wonderful. We love her, and we're just as lucky as she is. We're all in this together." She beams at me as we shake hands, and I walk to my car, sinking into the driver's seat with a satisfied sigh.
Saturday, July 24, 2010
Change of Shift, Vol. 5, Number 2
Wednesday, July 14, 2010
A Visit to the Doctor
"So, you're Mr. __________. Very nice to meet you. I believe your son is my patient, as well."
My client is solicitous, friendly and smiling as the doctor greets him. "That's right. Nice to meet you."
"You seem very healthy for a man of your age," the doctor says. "We should all be so lucky."
As we talk, review our client's history and relate our concerns and needs, the soft-spoken doctor listens----really listens----and reflects back to us what he hears. Performing a cursory yet thorough exam, he listens to our client's heart and lungs, prods his belly, inspects his limbs, checks his eyes, and otherwise gives him the once over with gentle and learned dexterity.
"I think you're all doing an excellent job caring for Mr. _________. He's a lucky man to have such a team looking after him 24 hours a day." He leans over and speaks very loudly into our client's ear. "You're a lucky man!"
Our client smiles broadly.
After the exam, the doctor recommends a tetanus booster and a pneumonia vaccine, and we're stunned when he comes back into the exam room to prepare and administer the vaccines himself.
"I'm sorry," I say, "but I've never seen a doctor give an immunization before. Do you always do this?"
He looks up at me as he flicks one of the syringes with his finger to remove any errant air bubbles. "Oh, when the nurses are busy I like to help out. It's no big deal, really." He leans down and administers the two injections deftly, one in either deltoid. Mr. _______ never flinches.
"Well, it's a big deal to us. Most doctors would never dream of doing such a thing," my colleague says to him as he places the used syringes in a sharps container. "You've been very kind and attentive."
"It's my pleasure, truly." The doctor shakes each of our hands once again, hands us prescriptions, referrals and a signed application for a handicap placard, and slips quietly out the door.
"That is one fine doctor," my colleague says to me, shaking her head. "What a positive experience."
We wheel our patient to the elevator, all of us quiet, knowing that we have just had what might be seen by some as a very unusual experience. The doctor was efficient, kind, thoughtful, thorough, paid great attention to detail, and listened to everything we had to say. As nurses, being really listened to by a doctor is simply a coup d'etat, and we left that office beaming with our collective good fortune.
A fine doctor, indeed.
Saturday, July 10, 2010
A Kind of Life
And so the days pass.
Recently, he was saved from a deplorable situation where he was taken advantage of by acquaintances looking for money or alcohol, rarely washed or bathed, and lived a life that most people would find appalling in its squalor. Now, living with family in the countryside, he is safe from ill-meaning neighbors and so-called "friends", yet he pines for that other life with all of his might. Stripped of his freedom, his drivers license and his car, he is at the mercy of nurses and social workers who mind his every move with a keen and earnest intent to help him stay clean, dry, well fed, hydrated and happy.
It is without a doubt that this individual was truly a danger to himself and at risk of injury or death without the proper intervention. Still, assessing his current situation, it's also quite clear that his quality of life leaves a great deal to be desired. We do our best to provide for him, keep him comfortable, and afford him some level of contentment. Still, it's so difficult to witness a person who seems to glean so little enjoyment from life, made even more keen by the sudden loss of his independence. Yes, it's a life, but how can we make it better? How can we bring him joy? And how can we make up for the changes that have stripped him of his ability to make decisions for himself? These are not easy questions to answer, and as we grapple with the possible answers, he stares out the window wishing that things had never changed.
Friday, July 09, 2010
Change of Shift Turns Five!
Happy 5th birthday to Change of Shift, and may there be many years to come!
Friday, July 02, 2010
Home Health and Hospice
My next article for Working Nurse (on the specialty of nursing informatics) will be published later this month, and in August I will be providing yet another article on the specialty of oncology nursing.
I am very grateful to Working Nurse Magazine for these opportunities, and am pleased that my writing career continues to flourish, even in these uncertain economic times.
Thursday, July 01, 2010
100 Blog Posts That Will Make You a Better Nurse
Thursday, June 24, 2010
Change of Shift, Santa Fe Style!
 Well, after a long hiatus, I'm finally hosting Change of Shift once again, and I'm happy to do so from the comfort of our new home here in Santa Fe, New Mexico! (For those of you unfamiliar with Change of Shift, it is a nursing blog carnival wherein nurses from around the blogosphere are featured in an "online magazine" that is hosted on a different nursing blog every two weeks.)
Well, after a long hiatus, I'm finally hosting Change of Shift once again, and I'm happy to do so from the comfort of our new home here in Santa Fe, New Mexico! (For those of you unfamiliar with Change of Shift, it is a nursing blog carnival wherein nurses from around the blogosphere are featured in an "online magazine" that is hosted on a different nursing blog every two weeks.) For those readers who are new to Digital Doorway, my wife and I sold our home in Massachusetts last summer, sold or gave away most of our things, bought an RV, and have been traveling the country for seven months and almost 10,000 miles in search of a new place to call home.
For those readers who are new to Digital Doorway, my wife and I sold our home in Massachusetts last summer, sold or gave away most of our things, bought an RV, and have been traveling the country for seven months and almost 10,000 miles in search of a new place to call home. For the moment, we've settled (perhaps temporarily, perhaps not) here in Santa Fe, New Mexico, and you can read about our travels here. That said, this episode of Change of Shift (that most venerable of nursing blog carnivals) will be peppered with photographs from around northern New Mexico for no other reason than the fact that they're nice to look at, entertaining, or simply a visual break from all of those pesky words that I'm making you read (unless, of course, you just look at the pictures!).
For the moment, we've settled (perhaps temporarily, perhaps not) here in Santa Fe, New Mexico, and you can read about our travels here. That said, this episode of Change of Shift (that most venerable of nursing blog carnivals) will be peppered with photographs from around northern New Mexico for no other reason than the fact that they're nice to look at, entertaining, or simply a visual break from all of those pesky words that I'm making you read (unless, of course, you just look at the pictures!). My thanks, as always, to Kim (of Emergiblog fame) for making Change of Shift a reality, and for putting nurse bloggers on the blogosphere map. Let's hear it for Kim (cue virtual applause, please).
My thanks, as always, to Kim (of Emergiblog fame) for making Change of Shift a reality, and for putting nurse bloggers on the blogosphere map. Let's hear it for Kim (cue virtual applause, please). So, without further ado, here are the participants in this week's edition of Change of Shift, Volume 4, Number 26..........
So, without further ado, here are the participants in this week's edition of Change of Shift, Volume 4, Number 26..........For whatever reason, it seems that lists are incredibly popular these days, whether it be for iPad apps or the best ways to darn socks, so here's a list of blog posts that feature lists about things that their authors think are worth our while to peruse........
At NursingSchools.net, we learn 50 things you never knew about babies (who would have thought that babies cry before they're born?); while over at The Health Harbinger, we are privy to 25 online startups that are democratizing medical data and information.
Speaking of iPad applications, CNA Class Online shares 5 Excellent iPad apps for "Dr. Mom".
And while we're talking about new technology, RN to MSN Programs submitted a list of 10 awesome Android apps for nurses (Android being Google's answer to Internet-based applications for cellular phones, more or less).
Sadly, we all do indeed need to think about the oil spill in the Gulf of Mexico, and NursingSchools.net submitted a sobering list of the 10 biggest health dangers behind the oil spill, which includes neurological disorders (and chemical sensitivity, I'll add) among the workers dealing directly with this toxic nightmare of the century.
 Thinking globally, The Health Hawk shares with us 17 intriguing infographics about global health, which, apropos of the oil spill, describes the fact that the average American driver uses 500 gallons of gasoline per year! (And we wonder why we're still addicted to oil?)
Thinking globally, The Health Hawk shares with us 17 intriguing infographics about global health, which, apropos of the oil spill, describes the fact that the average American driver uses 500 gallons of gasoline per year! (And we wonder why we're still addicted to oil?) And the lists go on.......
And the lists go on.......Aging Healthy submits a list of the top 50 aging and gerontology blogs for those of us who want to prolong our time on earth (oil spills or no oil spills....), and NursingSchools.net submits yet another post for our enjoyment and enlightenment, this time with 100 entertaining and inspiring quotes for nurses, one of my favorites being "Health is the state about which medicine has nothing to say" (W.H. Auden).
 And speaking of NursingSchools.net, we received yet another list (don't they work over there?), this time regarding the 100 best blogs for exploring alternative medicine.
And speaking of NursingSchools.net, we received yet another list (don't they work over there?), this time regarding the 100 best blogs for exploring alternative medicine.Moving away from lists towards actual prose (cue English teachers cheering in the background), we were happy to receive a submission from Barbara Olson of Florencedotcom fame, this particular piece on "Good Reads About Medication Misadventures" being recently published on Medscape (for which a username and password may be necessary in order to gain access).
And when it comes to those of us who might like a career change from direct care, Master of Health Administration shares with us "The Ultimate Guide to Health Administration Careers" (and the salaries don't seem half bad.......). Alternatively, Online LPN to RN delivers The Ultimate Guide to Nursing Agencies for those nurses who would like some assistance in landing their next job or plotting a career move.
Nurse Teeny at The Makings of a Nurse offers a very personal post about "transition shock" and a new job, something we can all probably relate to.
And over at Nurse Me, the author struggles with a situation wherein a patient's religious beliefs impact her ability to deliver the care that's needed in a post entitled Science vs Jesus.
 Author Peggy McDaniel at The American Journal of Nursing's Off The Charts blog chimes in for a post entitled "Protection or Harm----What Are You Doing at the Bedside?", and there is much sobering food for thought here vis-a-vis poor hand hygiene and hospital-acquired infections.
Author Peggy McDaniel at The American Journal of Nursing's Off The Charts blog chimes in for a post entitled "Protection or Harm----What Are You Doing at the Bedside?", and there is much sobering food for thought here vis-a-vis poor hand hygiene and hospital-acquired infections.In a post entitled "Fingerprints, Ad Nauseum", yours truly posits that there is utter bureaucratic insanity behind the need to be fingerprinted for every job application and license change that one must undergo (especially here in the Western US). Can't there be a central databank of fingerprints, or does the FBI just adore receiving multiple fingerprint cards for the same person over and over again? (It's your tax dollars hard at work, folks!)
And from the Land Down Under, Nurse In Australia shares a post entitled "Sheepish, Demure Nurses Pander to Inflated Egos". The nurse-doctor relationship is always something worth talking about, isn't it?

Our final two posts for this edition of CoS are well-written missives that address two very important issues worthy of our individual and collective attention.
First, Katie Morales of NursesNetwork.com (where my blog currently feeds automatically via RSS) discusses the legal and ethical notion of how companies profit financially with the use of our tissue and blood, whether we donated it willingly or not. In her post entitled "Not Much Has Changed, Katie offers several examples wherein companies benefited significantly from the cells or tissues of private citizens who then have no rights whatsoever to also benefit from the millions of dollars made from tissues harvested from their own bodies. What's the matter with this picture?
And last but certainly not least, our beloved Kim McAllister, the maven of Emergiblog and the creator of Change of Shift itself, delivers a passionate and convincing open letter to the American Nurses Association that rightly questions the ANA's refusal to endorse the creation of the Office of the National Nurse.
HR 4601 is an important piece of legislation currently making its way through Congress that would elevate the Chief Nursing Officer of the Public Health Service to the position of The National Nurse, a move that would bring nursing to the fore in terms of preventive health and the public's understanding of what nurses actually do. In March of this year, I wrote a blog post delineating how the National Nurse would benefit the country in myriad ways, and I invite you to read that post, read Kim's letter, visit the website of The National Nurse organization, and get involved in this important fight for recognition of nursing's rightful place at the American health care table.
Teddy Roosevelt once coined the term "the bully pulpit" to signify a position of authority or rank that gives it's holder the right and privilege to pontificate and share his or her opinions without reserve. While I hold little authority or rank in society as a simple nurse and writer, this blog is my own bully pulpit, and hosting Change of Shift is yet another opportunity to speak my mind and reach a larger audience, if only for a fleeting digital moment. I am grateful for your attention, and I urge you to contact your member of Congress about wholeheartedly supporting HR 4601!
 Thank you to Kim for this opportunity, thanks to those of you who are taking the time to read this, and a special thanks to the bloggers and writers whose contributions made this edition of Change of Shift what it is.
Thank you to Kim for this opportunity, thanks to those of you who are taking the time to read this, and a special thanks to the bloggers and writers whose contributions made this edition of Change of Shift what it is.And in the words of Garrison Keillor, "Be well, do good work, and keep in touch."
Tuesday, June 22, 2010
Fingerprints, Ad Nauseum
 Since coming out West, it seems that I can barely do anything at all pertaining to medicine or nursing without having to get my fingerprints taken.
Since coming out West, it seems that I can barely do anything at all pertaining to medicine or nursing without having to get my fingerprints taken.When I applied for my Texas nursing license, I obediently went to the local sheriff's department near my in-laws' home in Georgetown and had three FBI fingerprint cards done by a clerk who seemed relatively uninterested in the proceedings.
Six weeks later, I received notice from the Texas Board of Nursing that those prints were poor quality and unreadable (no surprise there), and was thus requested to have them done yet again. Since my wife and I were traveling at the time, I stopped into the court house in Silver City, New Mexico where a friendly but overworked sheriff's deputy expertly took my prints and sent me on my inky way. (Those prints were subsequently accepted and I received my Lone Star State license soon thereafter.)
Following my licensing fingerprint debacle, I applied to be a board member of a new medical marijuana clinic in northern New Mexico (they needed a nurse on the board), and of course, yet another set of fingerprints was demanded for the privilege of applying for membership. Still traveling, I stopped into the Sedona, Arizona police station where friendly volunteers happily collected my money and greased up my fingers yet again.
Now, having settled in Santa Fe, New Mexico, I have applied for several nursing jobs, and each of those positions requires a set of fingerprints to be sent to the FBI, and these sets were luckily simultaneously taken on an electronic machine that creates a digital facsimile that can be transferred to paper.
Maybe it's just me, but there appears to be an enormous waste of resources involved in sending multiple individuals for repeat fingerprint screenings ad nauseum. When one considers the human hours wasted, the gasoline burned, the reams of paperwork filed and the extraordinary effort and energy expended in the name of bureaucracy, perhaps there's some addiction to bureaucratic chaos (a la the Terry Gilliam film, Brazil) that precludes the powers that be (local, regional, state and national) from creating a central database in which each individual's fingerprints could be simply recorded once.
I'm sure there are those whose trust in the government has waned to the point at which even submitting to fingerprinting in the first place would seem absurd at best (and dangerous at worst), but since I've already allowed my personal information to be submitted to the FBI innumerable times, I would thus have few qualms allowing my prints to finally sit in an electronic repository for access by potential employers and others interested to know that I am indeed who I say I am.
With these latest sets of prints behind me, I have no doubt that I'll once again be visiting the state police or a local sheriff when the next demand for fingerprints rolls around. Til then, I'll give thanks that my spate of fingerprinting adventures is over for now, and my ink-stained digits can finally rest on their (positively identified) laurels.
Saturday, June 19, 2010
Jobs Galore
Now, after the byzantine process of obtaining my Texas nursing license (our permanent domicile is currently in Texas), jobs here in New Mexico themselves provide a plethora of hoops through which to jump in order to receive that first paycheck. From having to obtain yet another set of fingerprints to having to take several different exams to further (and unnecessarily, in my opinion) test my knowledge of nursing practice, obtaining employment as a nurse here in the Wild West entails a labyrinthine to-do list that threatens to eat up leisure time like there's no tomorrow.
Still, finding remunerative and (hopefully) satisfying work is very nice, and I'm grateful to have made it through the application and interview processes relatively swiftly. My new jobs should prove to be interesting and relatively well-paying (but less than my previous hourly wages as a nurse in Massachusetts), and I hope that the experiences are also fecund fodder for blogging and writing (with complete adherence to HIPAA, of course!)
Working as a nurse again will be interesting after such a long hiatus, and I look forward to writing about the experience as it unfolds, so stay tuned.....
Wednesday, June 09, 2010
Pounding the Virtual Pavement
Having never worked in a hospital, my specialty has been case management, home care, hospice and community health centers, so I am focusing my search on these professional areas. So far, there are several case management positions available in the area, and I surmise from my initial research and conversations with local Human Resources personnel that competition is indeed stiff.
While the nursing shortage appears to still be a nationwide phenomenon, I hear tell that many new grads are scrambling to find jobs after graduation, whereas many of us finishing nursing school in the early 90s had our pick of jobs before we even took the boards.
Many fellow nurses have told me over the years that not having Med-Surg experience is like committing professional suicide, severely limiting my access to well-paying jobs that are almost always in demand. However, having Multiple Chemical Sensitivity (MCS) makes working in hospitals quite dangerous to my health, taking into consideration all of the cleaners, chemicals, deodorizers, floor waxes and other industrial-strength products that are sprayed with wild abandon all over hospital units, ad nauseum. Thus, the field is narrowed not only by my lack of hospital experience, but also by my physical limitations.
Finding work here in Santa Fe should be interesting, and my hope is that something remunerative and part-time will manifest sooner than later, and regular paychecks will begin rolling in again as I don my scrubs and embody my nurseness once again.
Wednesday, June 02, 2010
Licensed by the Lone Star
Now that we will be suspending our travels and spending the summer in Santa Fe, New Mexico, it's time to look for work, float my resume, and translate that new license into action and income.
Some of you may wonder how I can work in New Mexico with a Texas license, and the answer is quite simple. A licensure compact exists between 24 states of the US, allowing for reciprocity between each state for nurses who hold a current license in one of those jurisdictions. With my legal domicile in Texas and my current (perhaps temporary) living situation in New Mexico, this licensure compact makes earning money and finding work much easier, a fact for which I am extremely grateful.
Having my new Texas license is a goal I have been moving towards for months, and I feel gratified that I have finally completed the lengthy application process. The job market for nursing positions is tighter than one might surmise, so having that license in hand is one of the important steps in enabling myself to pound the virtual pavement and find meaningful and remunerative work that utilizes the skills that I have honed for more than 15 years.
Stay tuned as the itinerant nurse searches for work in his temporary New Mexican home!
Friday, May 28, 2010
Change of Shift at "The Makings of a Nurse"
Friday, May 21, 2010
Nurses on the Run
My thanks again to Karen for including me in this exciting project, and please consider ordering a copy or asking your local library to do so!
Sunday, May 16, 2010
New York City Is Now a Home Birth Backwater
With one third of all pregnancies in the United States now ending in Caesarean Section, many midwives and supporters of natural childbirth feel that birth has become yet another cash cow for the American medical industry, with home birth becoming more rare (and less legal) as the decades pass. Some American cities and towns have even made public breastfeeding a crime, adding further insult to injury for women who choose natural childbirth and breastfeeding as a lifestyle choice in the interest of the health and well-being of their baby.
Despite the fact that home birth and midwifery are quite popular in other industrialized nations with advanced medical infrastructures (30% of babies in the Netherlands are born at home), the United States medical establishment still vilifies home birth as foolish and dangerous. In fact, the US has one of the highest rates of maternal mortality in the industrialized world (16.7 per 100,000 live births) as compared to The Netherlands' maternal mortality rate of 7.6% or Italy's rate of 3.9%. Amnesty International has even called the United States' childbirth track record "a human rights crisis".
With the current situation in New York City, home births are now illegal and midwives providing maternal care in the home do so at their own risk and without legal or medical support. As one of the most famous and progressive cities on earth, New York City has now become a home birth backwater, creating a crisis for the midwives and families who choose this natural alternative to the American medical industry's industrialization of childbirth.
Friday, May 14, 2010
Change of Shift at Muse, RN
Thursday, May 13, 2010
Everyone's Going to Nursing School
As older nurses continue to retire and the Baby Boomers enter their golden years, the demand for nurses certainly seems to continue unabated. Recent reports, however, indicate that a strained economy is forcing many nurses who used to enjoy part-time or per diem work back into full-time positions, making competition for jobs more challenging for new nurses entering the field. And with nursing schools overwhelmed with applicants and short on professors to teach those fledgling nurses, many would-be nursing students may turn to other allied health professions like Occupational, Physical, or Speech Therapy.
A recent article published in the South Florida Business Journal cites a new study by The Florida Center for Nursing which concludes that attrition from the nursing profession is far greater than the influx of new nurses. For example, in the last two years, the number of nurses in Florida increased by 27,000, however more than 50% of that gain was offset by nurses leaving the field, making the net gain of nurses around 11,000.
With more than 3 million registered nurses in the United States at this time, it's clear that the profession is still holding its own as one of the backbones of the health care industry. Still, with a shortage of qualified professors due to a large wave of retirements and few willing to replace them due to better salaries for clinical positions, all signs indicate that the overall shortage of nurses will continue to plague the United States---and most of the world---for some time to come.
In my view, geriatrics and long term care are sure bets for future nursing job opportunities, and those who are willing to pursue an advanced degree as Nurse Practitioners specializing in geriatrics will likely be readily employable in most regions of the country, especially those areas most popular with retirees.
I am thrilled that my cousin is pursuing the family legacy of a nursing career, and I pray that she will be accepted to the school of her choice and be readily employed upon her graduation. Still, one must be realistic that the calculus of the nursing shortage and the opportunities for employment have indeed changed since the days when new grads waltzed into jobs demanding any salary they pleased. Despite the shortage, competition for jobs is stiff, and the competition to get into nursing school equally as difficult.
For myself, having taken almost a year off for travel and writing, I am readying myself to look for a job in the Santa Fe area where my wife and I plan to spend the summer, if not the next year. While I may be fluent in Spanish and have a relatively impressive resume (home health, community health, hospice, and public health), I have never worked in a hospital and thus am somewhat limited in the type of nursing jobs I can pursue. I do not anticipate finding work to be overly challenging, but in the current climate, I realize that it may not be as simple as it once may have been. And with new grads flooding the market and willing to work for less than seasoned nurses accustomed to higher wages, perhaps finding the perfect part-time nursing job may be more challenging than I originally anticipated.
There's no question that nurses are highly trusted professionals who are sorely needed by an aging population. But in the current economic climate, can enough well-paying jobs be created for the seasoned nurses and new grads who are more than willing to don their scrubs and get to work? Only time---and economic forces---will tell.